Hey again everyone! Thanks for coming back to get the latest scoop. And thanks to all of you who have reached out telling me you’ve enjoyed the blog so far- I’m so glad that this is proving to be a good outlet for me as well as a source of information and answers to all of you who have decided to come along on this ride.
As is the case over the past few weeks, so many things have happened in such a short amount of time since I last wrote. In no specific order, I’ll try to touch on the bigger events and what they mean for decisions moving forward.
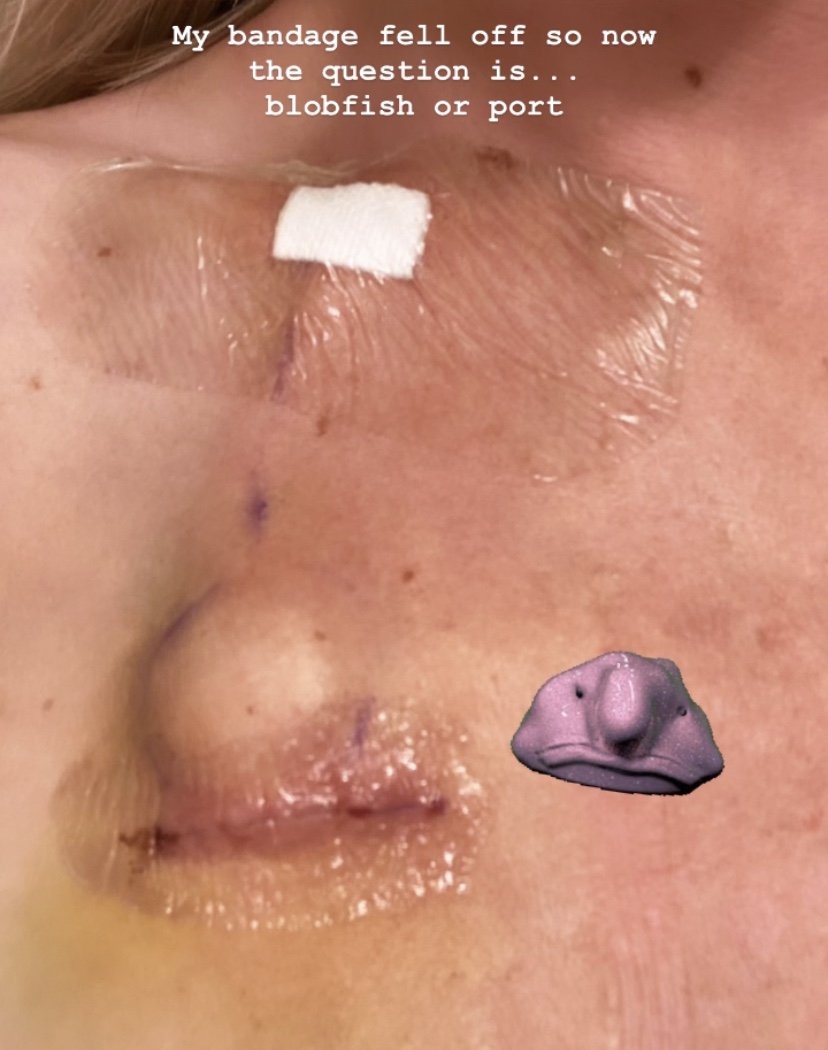
I completed four scans last week, including a nuclear bone scan, a CT, and two MRIs. I also welcomed Portia the Port into my life and sternum last Thursday, and she currently resembles a blobfish as she heals. I was advised by my oncologist to get the third COVID booster prior to starting chemo, so I did this on the evening of the day my port was placed. Let’s just say that was probably not the wisest idea. Friday was a rough one. But I made it through! And my antibodies are strong (well, for now).
As for the scans, most things came back clear (yay!), although I do have a large mass on my liver that we further investigated with an abdominal MRI (hence the two MRI’s; one was chest only and the second was abdominal). It turns out that I most likely have a benign tumor caused by Focal Nodular Hyperplasia (FNH), which is the second most common benign liver tumor and generally found in women of reproductive age. So, although the mass is decent-sized and not ideal, it’s basically what we call an “incidental finding”, which means, “when you go looking, you will find things.” …and we did (I have my wonderful friend Erin to credit for that statement…she warned me that they probably would, and that these things would most likely turn out to be benign). So, none of us were terribly worried and my oncologist suggested that we wait until after chemo to do a follow-up MRI to assess any changes. There have been no reports in the scientific literature of FNH masses becoming malignant, so this is mighty reassuring. Just one of those things that I’d probably never have known was there were it not for a full-body CT and MRI. Crazy.
The weirdest part of last week was definitely the port placement. I didn’t do any research going into it because I didn’t want to freak myself out, so I was under the impression it was just a casual incision and they’d stick something on me and tape me up and send me on my way. Welp, I was wrong. They got me set with an IV, rolled me from the prep room into surgery, and put me on oxygen and some benzos to take the edge off. They injected my chest with lidocaine and then talked me through their procedure as I was awake laying on the table. They made a small incision into the base of my neck and internal jugular vein, slid a catheter into said vein, fed it down into my vena cava (the large vein that carries blood from other parts of the body into the heart), made a larger incision right over my collar bone, shoved the port under my skin, attached the catheter to it, and then sutured and glued me up. We chatted the whole time and I barely felt a thing. What a trip. The first few days were really painful; I suspect it’s because they said my skin was really taut where they were trying to push the port in, but the pain may also have been enhanced due to the booster shot. Portia has been healing well since then and I’ve been able to get a few decent workouts in, including a run, which has been great. It basically just feels like I have a giant button hiding out under my skin and a weird tube inside my neck and chest. Which, I guess I do.
So, moving onto this week…my parents were here which was AWESOME. They’re such saints. They are so active and busy all the time at home, you’d think they’d want to come visit relax, but nope (anyone who knows me well knows that this is nearly impossible for my family). The very first thing they decided to do was to clear out my storage garage in order to create space for an area where I can have a stationary bike stand and use my road bike for workouts during chemo. This was an idea suggested to me by a friend who went through all of this over the past few years and loved having the ability to use her bike and the Peloton app to do rides with friends on her infusion days. So, I’m hoping to do something similar and use this space as a little workout getaway, if even for a recovery ride or something relatively low-key on the days where my energy is really low. Photos of this space to come! It’s amazing what they’ve done in just a few short days. They also helped improve my little zen garden out back which is one of my favorite parts of this whole property. I am so lucky to have them!
My mom came with me last night to a meeting with my oncologist to review the scans and confirm steps moving forward. I’m so glad they got to meet, as my oncologist is quickly becoming one of my favorite people. She’s super kind, yet straightforward, patient yet concise, and so incredibly knowledgeable about this whole process. She showed us the MRI of the tumors and my lymph nodes, which was pretty cool to see, and she advised that I do get a brain scan this coming week since breast cancer does sometimes metastasize to the brain and I’ve been having some minor headaches recently. We assume it’s just due to stress and lack of sleep overall, but she wanted to cover all our bases. She also brought up a slightly strange finding on my CT that showed mild atherosclerosis of one of the coronary arteries in my heart. Since this is not super common in my age group, and generally not found as commonly in people with a lower BMI, we talked about family history of heart disease (my grandmother had a valve replaced and my grandfather had a heart attack later in life) and she wants me to get a lipid test done just to be sure this isn’t something we need to be overly concerned about. So, I’ll have that done on my first day of chemo prior to getting any of the drugs. At the same time I’ll also get tested for a clotting disorder called Factor V Leiden, which is in my maternal family. So we will see what all of these results show and go from there.
Brandon and I also had a meeting with a surgeon this week which went really well, but definitely opened up more questions in terms of the type of surgery I’ll pursue. A lot of it will depend on my genetics test results, which I’m hoping come back this week. If they are positive, they’ll 100% recommend a double mastectomy. If they are negative (i.e. if I don’t carry any known gene mutations for the genes that predispose to breast cancer), then most surgeons/oncologists lean toward doing a single mastectomy since there is no scientific evidence showing that removing the healthy breast decreases chance of cancer occurring in that area. Additionally, since my white blood cell count will be super low at the time of surgery due to 6 months of chemo (aka I’ll have no immune system), some surgeons and oncologists feel that it is not worth the infection risk to do the double mastectomy when the chemo-wrecked body will already be fighting so hard to heal from the removal of just one. They can then come back after radiation is complete and do reconstructive surgery using an expander, an implant, or your own tissue (your own muscle from your back- your lat! Or your stomach! It’s crazy!), and then make it all symmetrical and cosmetically matching the other side (minus the scars and such). Again, many of these decisions will depend on how my genetics come back, and don’t have to be made for another few months, but I thought it was all really interesting so I wanted to share. I won’t even get into the mess of the lymph node surgery portion of all of this and how they decide how many of those come out…those fine details can be left for another time (aka, it’s complicated).
The last and final thing I’ll tell you about from this week is the ChemoTeach. This was essentially a meeting with the nurse practitioner who switches off with my oncologist from week to week when I go in for my transfusions. She reviewed the first half of my chemo protocol, the drugs A & C, which stand for Adriamycin (some might know this drug as Doxorubicin) and Cyclophosphamide. We talked about how the drugs work (both inhibit DNA replication of cells), how they’re given to me, and what the side effects will most likely entail. Let me tell you- this is going to be FUN! Bone pain, constipation, nausea, nail changes, hair loss (womp womp), bladder irritation, acid reflux, mouth sores, fatigue, dry mouth, reproductive and hormonal changes, possibility of heart irregularities and shortness of breath. I’ve never been one to get weird about side effects because I know they always list them ALL and generally most people don’t experience the majority of them, but unfortunately in this case it sounds like these first two months of the AC protocol I’m almost guaranteed to experience most (except, hopefully, the heart and lung stuff). BUT I am hoping to stay as active and busy as I can, take things to alleviate side effects (who woulda thunk that Claritin can help with bone pain because of the reduction in histamine release?!…wild), and try to stay on top of things through integrative therapies and nutrition. Luckily I’ll have bi-weekly check-ins with the nutritionist and my oncologist between infusions to see how things are going and see what type of adjustments we need to make. I’ll also have bloodwork done every single infusion day to check my white blood cell count and other parameters to ensure that I can receive the chemo drugs on that day. These first 8 weeks I have AC infusions every 2 weeks, and apparently energy levels dip really low days 3-7 or 8 (as well as white blood cell count) and nausea tends to be the worst from days 4-7 or 8. Those, as well as bone pain, are the main things I am definitely not looking forward to. After the completion of the AC rounds, I will have a two-week chemo break before beginning the next three months of chemo, which will be other drugs (T, H, and P) I’ll go over with my oncologist when that gets closer. So for now, I guess we will just take it week by week and see what happens. Thank goodness for the cutest handmade pill box of all time from my friend Kristy!

The fun begins! 
One last item, because I have to end on a good note! Yesterday, I was extremely honored and happy to have been offered the opportunity to co-author a scientific manuscript focused on a case study from one of my recent externships. I am super excited about this because it’s one of my favorite species, a case I felt very invested in, and the people I’ll be authoring with are wonderful veterinarians and colleagues. This was definitely a huge highlight of the week and I hope to be able to help write the manuscript over the coming months during treatment.
So, to recap: chemo starts this coming Wednesday, 9/15 (and my sister is here this week, yay!), I have one scan left (for now), which is a brain scan, this Friday, and a few different blood tests for lipids and clotting disorders.
Whew! That was a lot. I can’t believe how many things are happening every day. The hours just fly by, but I am trying to remember that now more than ever each day is a true gift. Please keep that in mind as you go about your week, and know just how appreciative I am of each and every one of you being here, being interested, and being a part of my life. Signing off for now and sending love and doggie kisses to all of you.







Amanda- I just love your upbeat positive attitude about what is happening to you! That’s half the battle I think! I’m so sorry you are having this experience in your young, active, busy life. But I’m glad you have done all the research and have a strong basis and understanding of all that’s happening. Love the workout room in the garage for you! Bless your sweet mom and dad (and greet them from us)!
LikeLike
Hi Amanda, Glad getting started went quickly for you. Waiting can be the worst. Yes the side effects list is so long but it doesn’t mean we get them all. I had very little nausea and the pills I had helped the few times I did. Yes the Claritin is a game changer for the bone pain! My biggest issue was fatigue and loss of appetite. But now 8 months later chemo, surgery and almost all my radiation is behind me. Keeping you in my thoughts and prayers that your journey also goes quickly. Mary Rose
LikeLike