Sliced n diced, slashed, cut, hacked, split, slit, or severed. Any of the above descriptors would probably work to describe how my body feels at the moment. It’s been one week since my double mastectomy and axillary lymph node dissection, and oooo dawggie it’s been a trip. Yesterday was the first day that I’ve felt about 75% independent in that was able to take a (semi) long walk by myself, can now cut food and prepare meals on my own, can reach upwards at about a 60 degree angle above my head and can do simple things like make my bed, fold laundry, etc. I still can’t hold the leash to walk my dogs (in case they pull or make a sudden movement sideways), so my parents were still walking them for me while I walk alongside as of this morning, and Brandy and Alyssa will help with me the same for the next few days. Before I dive into the details of the surgery, pathology and recovery over the past week, I have to say a giant, extreme-sized, enormously huge THANK YOU to my amazing parents for taking such excellent care of me and the monsters this week. They have been incredibly helpful and have been to my place 3 times a day, if not more, every single day to walk the dogs, help me with my drains, take photos of my incisions for monitoring, help log my meds, prepare meals, and comfort me during any menty b’s (only one menty b so far in recovery, so I’ll take that as a win). They are the absolute best and I am so so incredibly lucky to have them.


Also a giant thank you to Brandy for being there for me from 5 am on surgery day to when I woke up that evening, then delivering an exhausted and loopy me the following day to Fort Collins and showing my mom how to take care of my drains as I was pretty much still in an anesthetic stupor. Also, thanks to my big brudda for picking me up in FoCo to make the drive down to Anschutz for surgery and to my sister and vet school friends for organizing and being on deck all week in case we needed extra help with the doggies. I am so lucky to have such an awesome team of helpers! I am so so so thankful for all of you.
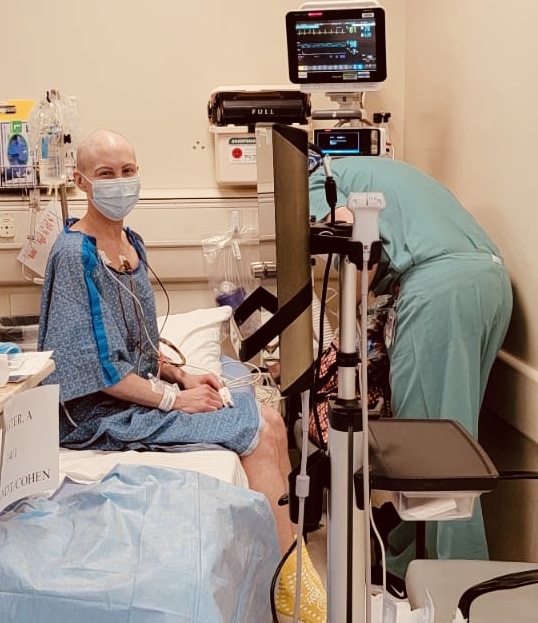
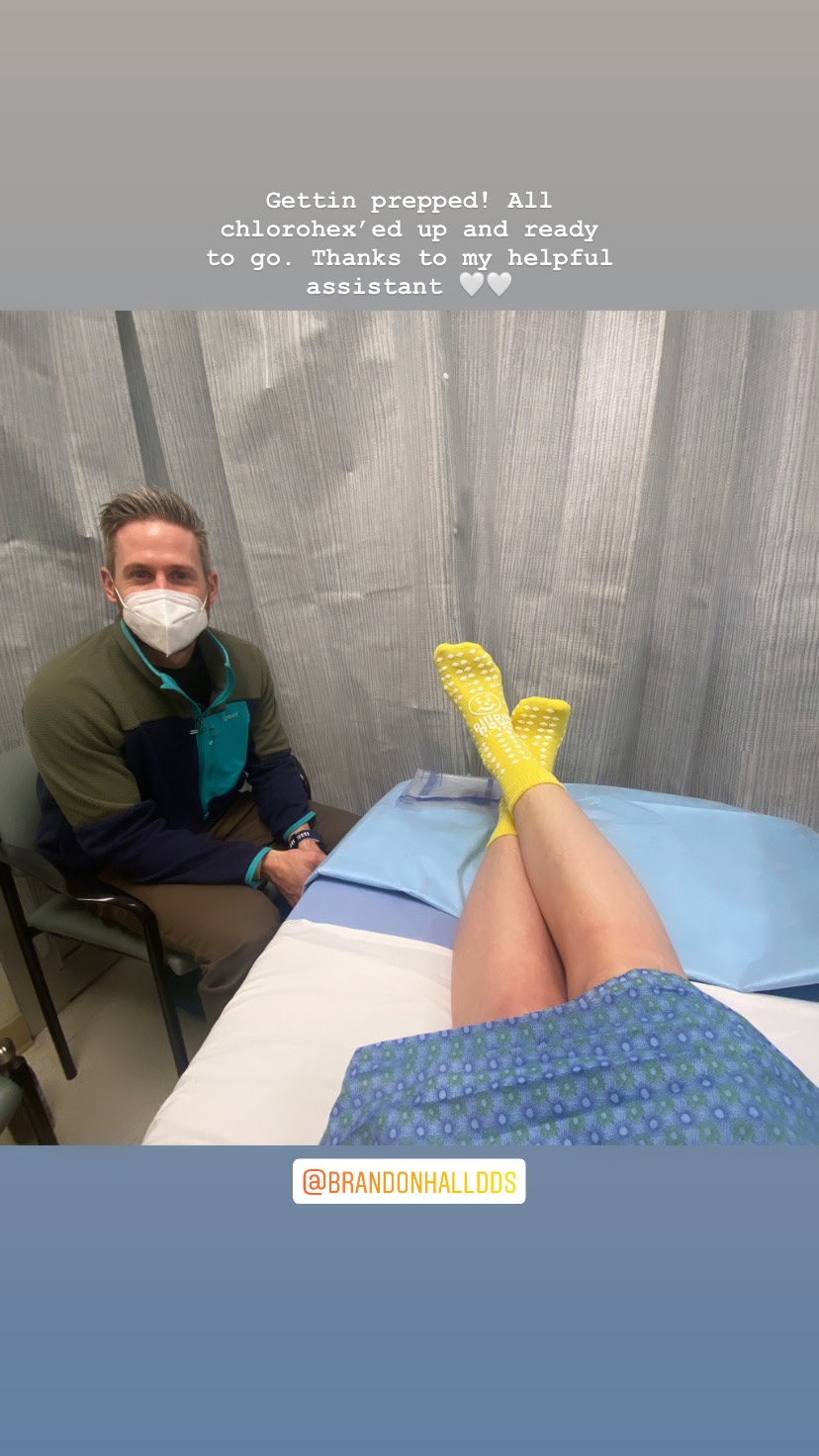
Ok, so onto surgery day. We checked in at 5:30 am and my surgery began right around 8 am. There was tons of prep beforehand and I even got to experience a bilateral paravertebral block (pictured below- I asked Brandy to document as I thought it was pretty cool). My surgeons (Dr A & Dr C, “deconstructive” and “reconstrcutive” surgeons, respectively) both came in just prior to surgery to say hello and to ask if we had any last-minute questions. We didn’t, but since I was feeling a little loopy on feel-good drugs already I decided it was appropriate to tell my female surgeon (Dr A) that I thought she had beautiful eyes and her scrub cap really brought them out. Pretty sure I probably told her that eight more times in the recovery room, but that’s neither here nor there. Anyway, they wheeled me away and I kissed Brandy goodbye in my cushy yellow hospital socks and party hat (aka surgical bonnet) while chatting to the anesthesia team about dogs (what else) and all I remember after that is seeing the surgery suite, realizing how many damn people it takes to do the surgery I was about to have, and seeing them wheeling basically a meat hook looking contraption toward me that I realized my arm would probably be hanging in for the next 6 hours. They put my mask on and I was out like a light.
The surgery took about 6.5 hours and then I recovered for about 2 hours before they wheeled me to my overnight room, which basically consisted of two thin walls and a curtain between me and the hallway. I remember peeing in a bed pan at some point and thinking I was hilarious when the nurse asked me my boyfriend’s name and I said, “Brandon, but he prefers Brandy.” She understood the assignment, so she actually wrote that up on the window and I was very pleased with her and myself. Soon after that I saw Brandy’s cute little face pop up in the curtain and I said, “Dr. Brandy!” and then I think I just talked in anesthetic loops about weird stuff for the next 30 minutes or so. I also promptly told him that the patient in the room next to me was “very loud” and “very extra” and that her TV was really annoying (she blared it all night long, so to be fair I was not making this up. She was VERY extra). Nurses came in and out for the next few hours and checked on my pain levels and drains (and taught me how to “milk” and empty them (barf)) and it was all a little blurry and goofy for awhile.
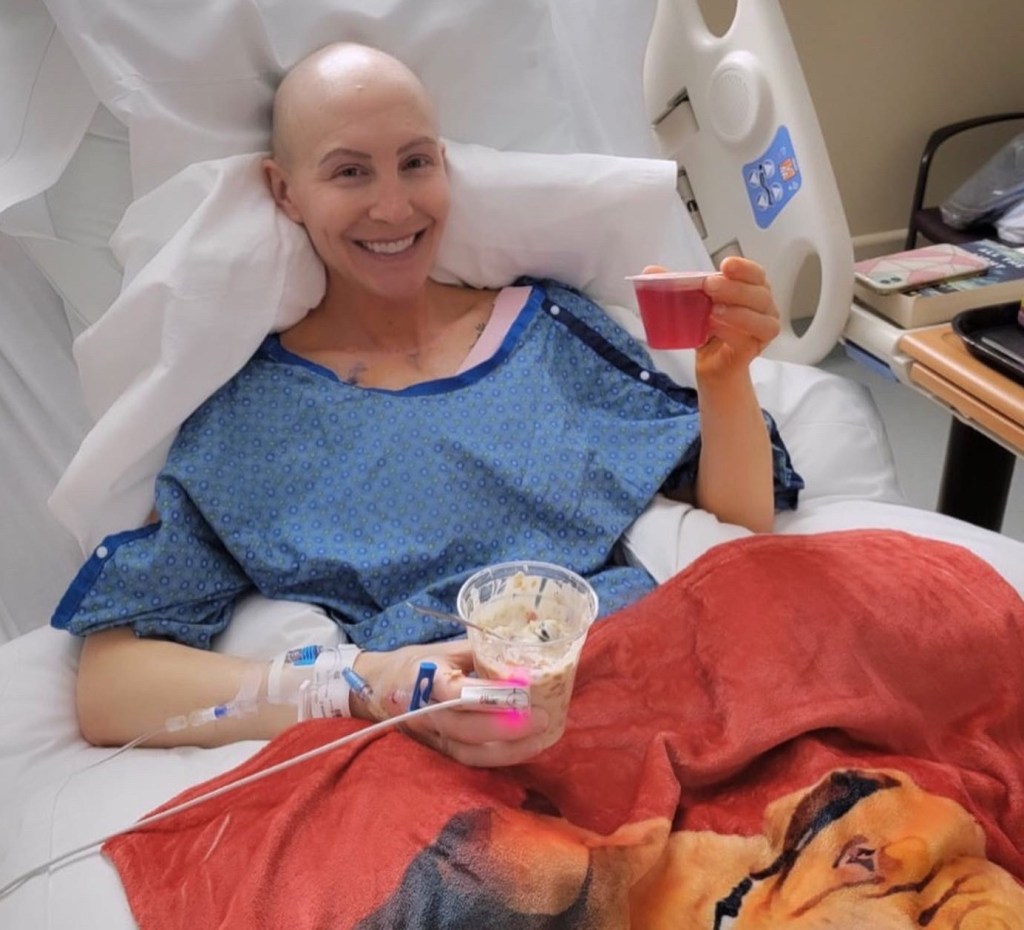

I ate some yogurt which tasted amazing and Brandon sat on my bed and hung out until it was time for visitors to depart. He told me later that I looked like a frail little sick grandma when he walked into the room and it was the first time it really hit him just how sick I really am. He was right- I looked like total shit and my body was hardly able to move so I don’t blame him for being a little shocked. I was white as a ghost and could barely get out of bed without assistance, so I certainly felt it. I spent the night laying awake with these anti-clot puffer things constantly pulsing around my lower legs and the bed moving up and down automatically every few minutes and the patient next door’s TV roaring Jerry-Springer-like shows all night long. I stared at the wall clock for hours waiting to fall asleep but it never really happened. I ended up making friends with one of my nurses who told me all about her adorable rescue dog, Ragner, who was a bait dog in fighting rings and incredibly fearful, but now the love of her life. She even gifted me his photo from her desk to aid in my recovery so I ended up staring at his face from about 2 am-4 am until the hospital started to wake up again. That nurse and Ragner were definitely a light amongst the dark parts of that first night.



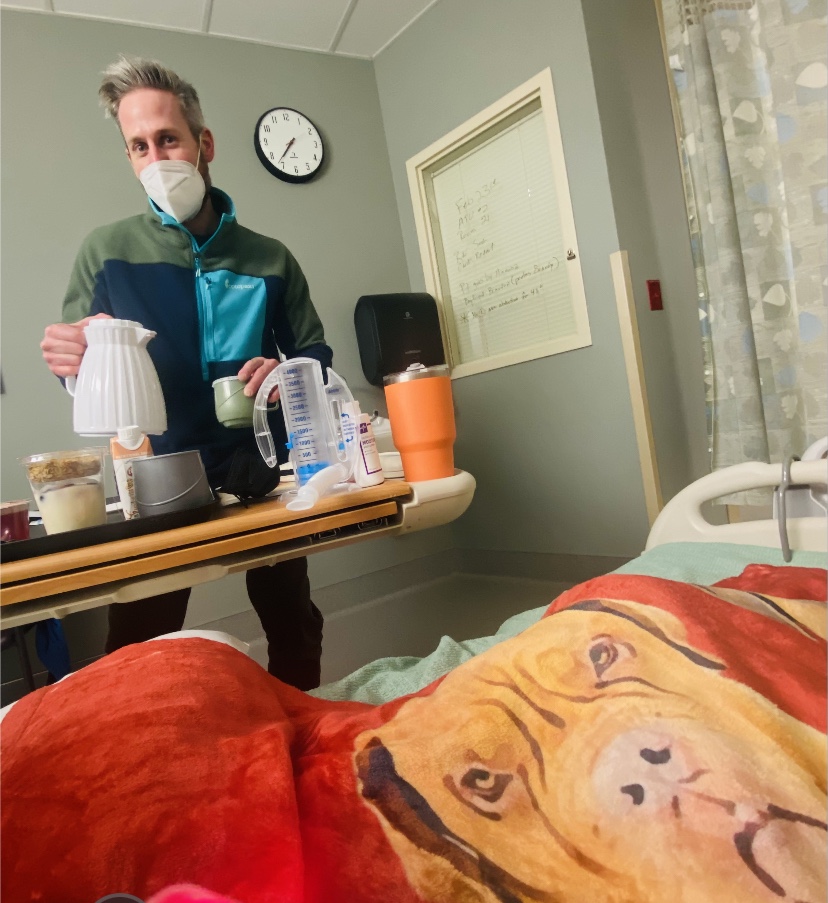
Brandy returned in the morning to scoop me up, and after some more pain meds, a visit from the anesthesia team to make sure things looked ok, a hug goodbye to my sweet and funny nurse Sue, and some help getting dressed, they wheeled me out and we were off to Fort Collins. My mom was here to receive me and amidst some very excited doggies we managed to take care of my drains as a team and then get a first look at my incisions. I must say this was definitely a different experience than what I imagine a first look at a wedding would be. Quite the contrary, I would assume. I undid the tight pink Velcro bra they had strapped onto me and opened my shirt with the drains hanging out the sides and looked at Brandon and my mom’s faces as they saw my post-mastectomy body for the first time. They both looked a little shocked, but surprisingly calm, so that was reassuring. I think they were both surprised at how little bruising I had, but also realized in that moment just what my body had undergone. I couldn’t quite look at the incisions yet on day one, but was able to take a look the next day in photos. We started taking pictures right from the start in order to monitor the incisions for infection and healing, and it’s been interesting to see the changes that have happened in just one week.
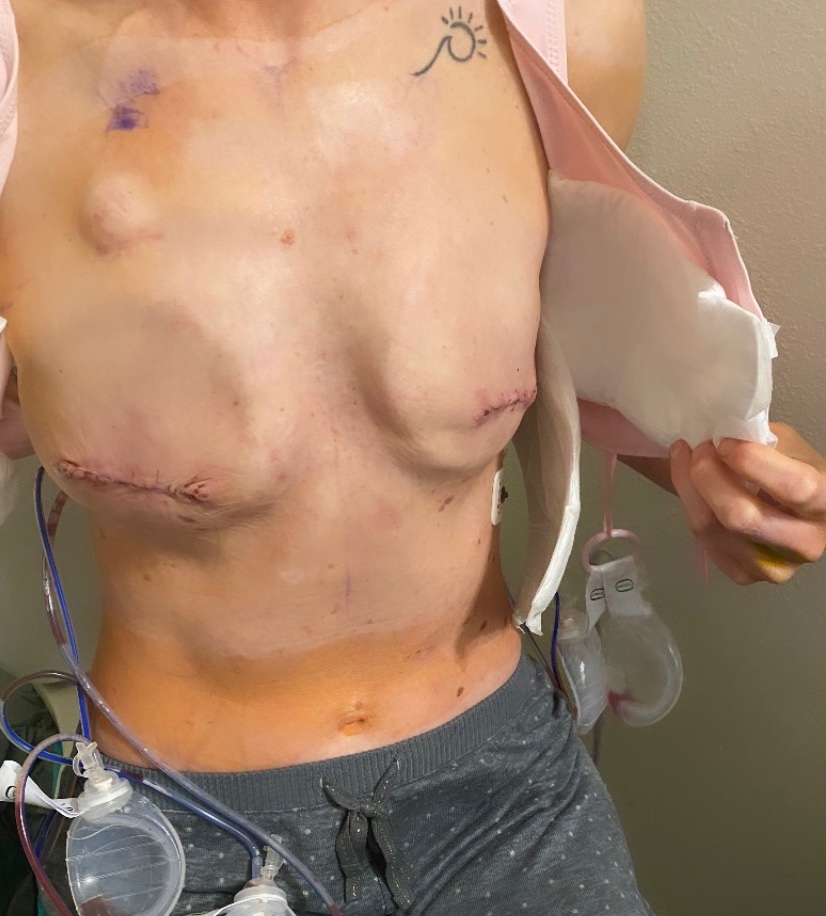
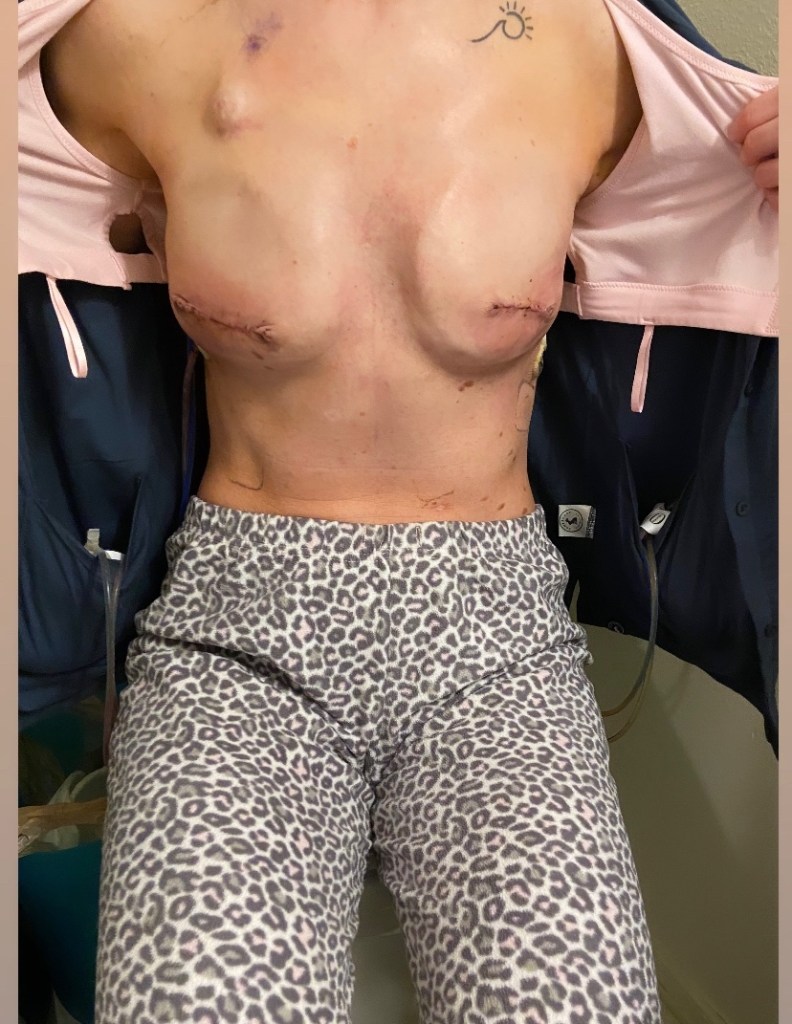

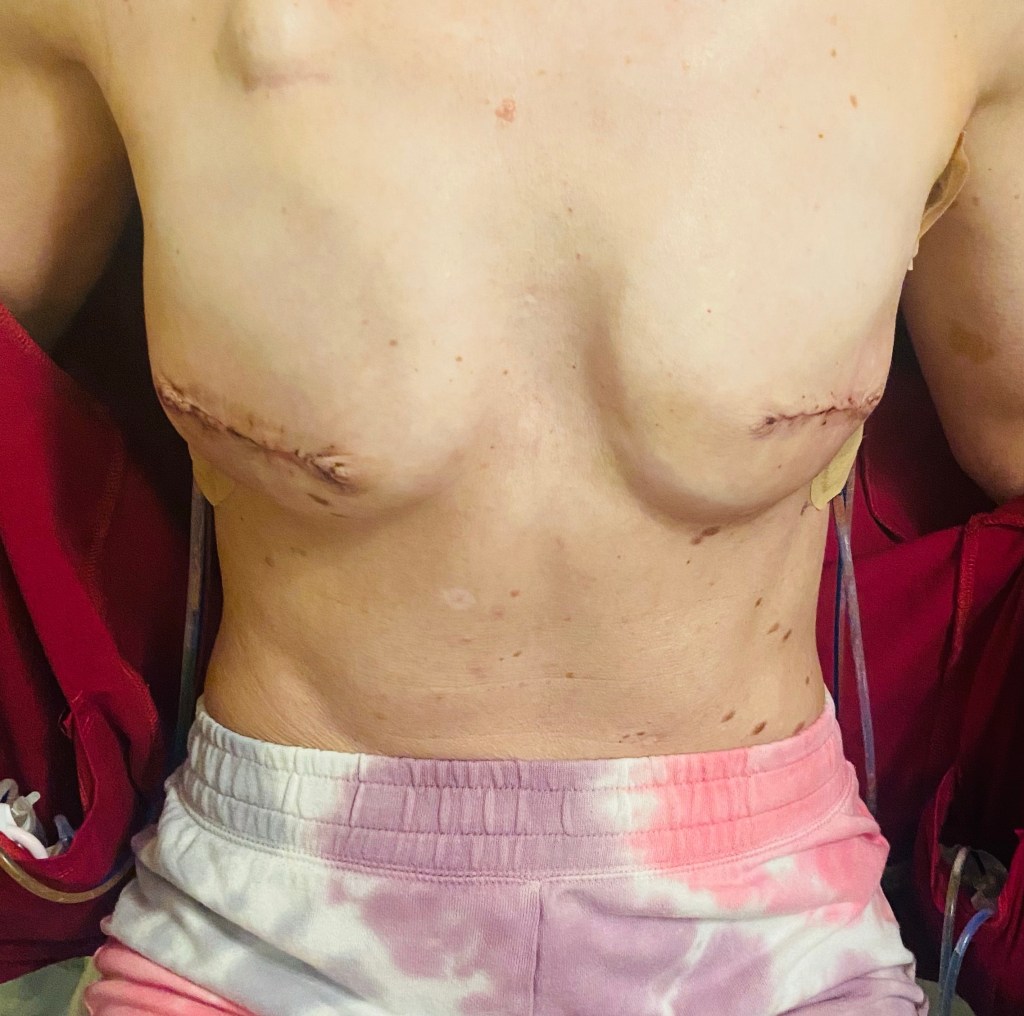
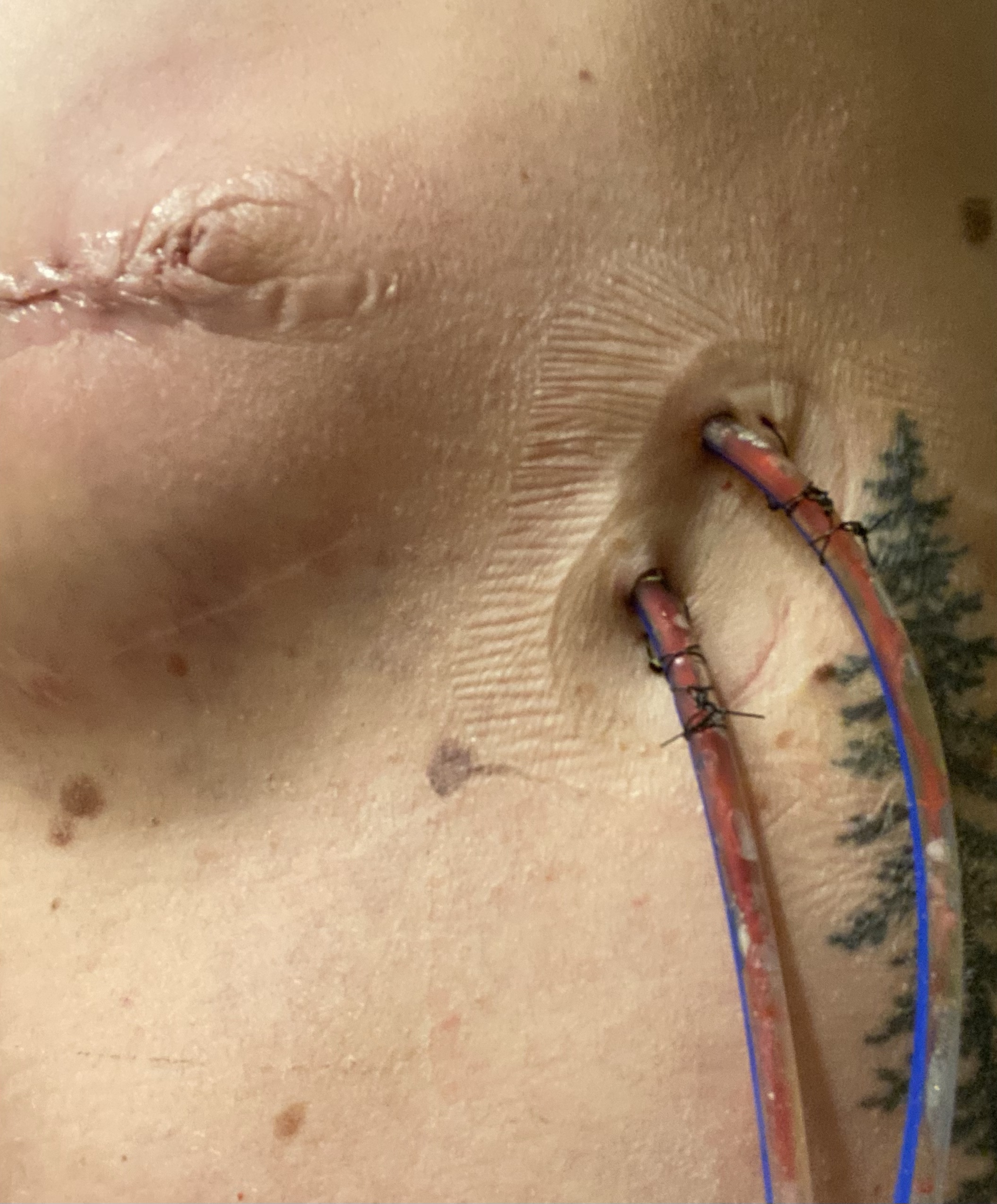


Ok, so about the surgery itself…I had both breasts removed, as well as an axillary lymph node dissection, which basically means they went in through a big incision just below my left armpit and they took out a few of bundles of lymph nodes embedded in fat. All in all they removed 15 nodes, and 3 of those nodes tested positive for cancer. One of those positive nodes was within a bundle of “sentinel” nodes, which is the first bundle that the lymph would travel to from my breast, and the other 2 that tested positive were in bundles just beyond the sentinel nodes. When they removed my breasts, they removed all the breast tissue and my nipples, as my tumor was close enough to my nipple that there was a chance that the nipple could have retained cancer cells, and could grow cancer later on had I kept them. So, for this reason, I decided with the guidance of my surgeon to have a “non-nipple sparing”, or what they call “skin-sparing” mastectomy. Aka- the type of mastectomy with the large scars across the mid-section of the breast. Because my tumor was in my left breast and ran from behind my nipple up along the outer edge of my breast and into my axillary region, and was located quite high up, my surgeon explained that she would have much better access to removing all of the tumor if she could go in through the center of my breast rather than from below. That was all I needed to hear in order to decide to give up the nips. On the right side, they removed all of my breast tissue and nipple as well, but since they didn’t have a reason to need to access as high up in order to remove a tumor (as they did on the left), the incision is lower. In the end, these scars should heal well and blend somewhat with my skin, and they will even things out as much as possible once I have reconstructive surgery next year. After I heal from that, I hope to get some cool tattoos that incorporate my scars (I have a few mastectomy artists in mind, and love the work done in the photos below by an artist that I follow in Chicago).


The type of cancer that I have did not change from my original biopsy done 7 months ago, which was “Ductal Carcinoma In Situ” and “Invasive Mammary Carcinoma”. The cancer came back as “triple positive”, meaning that it is receptive to the hormones estrogen and progesterone, and it overexpresses the HER2+ protein. The only difference from my original diagnosis is that they did not find that one of the tumors was HER2-, which they had found previously. I’m not sure what this means in terms chemo moving forward, but I should know more after next week. I don’t anticipate that it will change the treatment plan, since I have always had at least one portion (the larger part) of my tumor growth that was triple positive.
One crazy thing I learned this week is that chemotherapy apparently doesn’t touch the cancer that is “in situ” (aka “in place” in the milk ducts), only the cancer that invades other tissues and that you feel as an actual lump, so although on imaging my tumors had decreased in size by quite a bit, there were still 8 cm’ worth of “in situ” cancer in my milk ducts and 2.4 cm of the “invasive” type as a tumor found in my left breast tissue (this surprised me! I did not know this about chemo until they explained it to us yesterday). So, basically if you feel a lump you are not feeling the “in situ” cancer, 99.9% of the time it is the “invasive” part of the cancer that has invaded other tissues outside of the ducts that you can feel. My right breast had no tumors and all tissue appeared to be benign on pathology (this was expected as nothing was seen on mammogram at time of my original diagnosis).
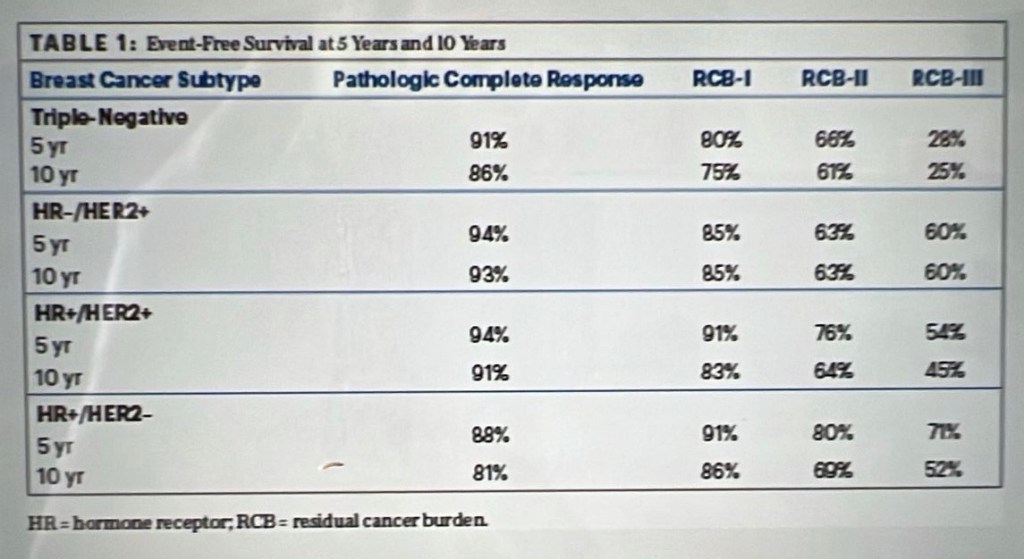
The other interesting part of the pathology report that is worth mentioning here is the “Residual Cancer Burden” calculator (from the MD Anderson Cancer Center) that is used to compute the Residual Cancer Burden:
“Residual cancer burden (RCB) is a continuous score that captures the amount of residual cancer after neoadjuvant chemotherapy and predicts disease recurrence and survival across all breast cancer subtypes. Six variables are included in a calculation formula. The calculated RCB index value can also be categorized as one of four RCB classes: a value of 0 equates to a pathologic complete response. The following three classes: RCB-I (minimal burden), RCB-II (moderate burden), and RCB-III (extensive burden).
This link brings you to a very readable and easy-to-interpret article summarizing the details and prognoses associated with RBC: Residual Cancer Burden is Prognostic of Outcomes. Based on primary tumor area, percentage of the tumor that is invasive cancer, and the extent of lymph node involvement, I fall into RBC-II (moderate burden). The text within my path report that specifically reports this says:
“Grossly we measure a 5 cm by 3 cm densely fibrous area consistent with a tumor bed; histologically, we find invasive tumor throughout this entire area. The tumor is variably cellular within this tumor bed with an overall estimated cellularity of 10%. Incorporating these figures into the Residual Cancer Burden Calculator from MD Anderson Cancer Center, we compute a residual cancer burden of 3.175, which provides a residual cancer burden class of RCB-II”
Had one more lymph node been positive for cancer, I would fall into RCB-III (I only know this because my surgical oncologist explained it to me and because I used the calculator, found here): RCB Calculator. So, not great, but pretty much what I was expecting (and I am glad that my primary oncologist prepared me for this).
The lymph nodes removed were quite a few, which is not ideal for chances of lymphedema, but they did a cool procedure called a “lymphovenous anastamosis” which helps reduce my chance of lymphedema by up to 30%, so I am really grateful for that. My reconstructive surgeon (Dr C) did this portion, which entails suturing my lymphatic system to a vein (with a teeeeny tiny suture) so that the lymph has somewhere to go. It is a relatively new procedure but they’ve had a lot of success with it, and he was willing to take the extra time to do it, so I was very excited when they offered it as part of my surgery.
Ok, so the recovery portion. The weirdest and most difficult part right now is the numbness and tightness from my left axillary region to the middle of my left tricep area. It’s basically numb and/or feels very bruised in different sections, and I may not regain full feeling along the back of this arm. They are having me start doing light massage a few times a day to the tricep area with hopes I may have eventual nerve regeneration in that region (massage is painful but manageable right now). I can’t extend my left arm fully forward yet and only can really touch the top of my head. I can reach behind my head slightly and can do small arm circles, but it will take quite a bit of time and physical therapy to regain full range of motion and mobility and strength in my left arm. I can’t feel any of the incisions (either on my breasts or under my axilla on the left) but I can feel the center of my chest and around the lateral edges of the expanders. Everything feels very tight and stapled, but the pain is mostly gone so long as I don’t do any sudden movements and don’t extend my left arm past certain points. The first few days were pretty painful and rough, but I only had to take the Percocet for about 3 days so it wasn’t too terrible. The drains are clunky and itchy and annoying, but all in all not too bad now that I am down to two. I had two removed on Thursday at my recheck appointment and have two remaining (I will include a video below of one of the drains being removed for those who want to watch- kind of cool). Once these are out I will start to feel a lot more free and able to do most “normal” things again (besides intense workouts) for a few more weeks or things that put a lot of strain on my axillary region or pectoral muscle area.
For the reconstructive part, Dr C placed expanders under my pectoral muscles that are basically like really stiff fillable round containers/pockets that will be filled with saline each week starting this Monday (for four weeks). They injected 100 cc’s in at the time of surgery and will fill them with another 300-350 cc’s of saline slowly over the coming month to allow my skin to stretch to accommodate the eventual implants they’ll put in when they take the expanders out. The expanders are sutured into my chest wall and will be exchanged for the implants in about 9-12 months, depending on how I heal from radiation.
Radiation will begin in a few weeks, after I meet with my oncologist to discuss next steps next week. I will have to get little placement tattoos for radiation and will be going to the cancer center here in Fort Collins Monday through Friday for 6 weeks or 33 sessions of radiation. It will be applied to my left breast and left axillary region, and sometimes extends a bit up the neck. During this time I will begin PT for my arm and chest (and whole body) as well as start a new more mild form of chemotherapy and continue immunotherapy to try to eliminate any remaining cancer cells in my remaining breast cells and lymph nodes. I will also start on ovarian suppression drugs (Lupron) in order to keep my ovaries from producing estrogen until I can get a total hysterectomy at the time of my reconstructive surgery. My ovaries have been turned off because of the more intense chemo I was on, but they will start to wake up again soon, so the Lupron keeps my estrogen levels low so that I have less of a chance of cancer recurrence, since my type of cancer is fed by estrogen. One weird thing I noticed this week is that my hot flashes have been less intense, and we think it’s just because my body was in such shock from the surgery. They were gone for about 3 nights (and it was amazing), but they have come back over the last 4 days or so. Gotta love hormonal fluctuations! Always a blast.
In terms of recovery, they told me the first two weeks are the hardest and I should be mostly healed by 4-8 weeks (I am hoping closer to 4 weeks). I feel like the worst part has been the post-anesthesia bloating and fatigue, and just the annoyance of having to sleep upright and empty the drains 3x a day. You have to strip the tubes of the tissue and blood inside of them and push it all down into these flexible plastic bulbs, which then are emptied into cups to measure the total output. Once the output is under 30 mL per day, they’ll remove them. So on Thursday, since two of my tubes were below the output, they were able to be removed (hallelujah!) and I am hoping the other two might be removed this coming Monday. My mom helped me do this task for the first 4 days after surgery, 3x a day, which is truly a heroic effort considering just how gross and tedious of a task it is.
The fatigue is lessening now that I am off of the Percocet and able to go for longer walks. I am sleeping decently well, not great but not terribly, so that’s not been as big of a challenge as I expected. My dogs have been so sweet and comforting and patient as I had to spend the first few days kind of lazing around, which they’re not used to. My parents walking them has helped us all SO MUCH, and it’s helped me to get out and get moving as well. It’s helped a lot to get back on a more regular schedule again and do three walks a day with Spanish and other computer tasks or projects in between. I feel like the days are going by fairly quickly now that I can move around a bit better and it has helped me mentally as well.


Emotionally I am up and down. Overall I feel like I am staying as positive as I can, when it feels like I am able to be. When I feel down, I let myself feel down, and I had a good cry with Candy V the other night which was cathartic. I am just so sick of this cancer crap and it feels like I’ve been living this nightmare for a really long time now. I am trying to be patient and stay the course, but sometimes it’s hard. I see all my friends and classmates and family and partner continuing their lives as normal and accomplishing goals and moving forward, and I feel like I am just in this weird in-between limbo that I can’t get out of. I know I have to continue to battle as hard as I can, and eventually I’ll get there, but sometimes when I think about the daunting road ahead and the chance of recurrence I get overwhelmed and pretty down about it. But, at this point there’s no other choice for me but to push on and keep doing the best I can to get through this.
As for right now, the next big thing is a PET scan this coming Wednesday to determine whether or not the mass in my liver is cancer. I am pretty nervous about this appointment but trying not to get too in my head about it. I am feeling hopeful that this will be some weird benign growth that we can take care of relatively easily and it won’t continue to be an issue. But, that is to be determined in a few days, and for now I will just focus on continuing to heal, walking, and getting stronger.
I will keep updating with the reconstructive photos as I go, since I’ve had a lot of people reach out about the whole process and how it works. Even though it’s terrifying and surreal having it all happen to my own body, it’s also fascinating to me. I hope documenting all of this continues to educate and inspire those of you who have chosen to follow along and who have reached out with kind words and appreciation. It means more to me than I can express in words and I am eternally grateful for all of the support and love. Sending love and doggie kisses to all!

On behalf of your fans, we are so proud of you! I can’t begin to think about the procedures that you go through. So glad somebody is there to hold your hand. One hopeful sign is that in all of those pictures you never seem to lose your smile. Keep it up! And I am not a fan of tattoos but, yeah, I could see some really great ones like you offered in the post.
LikeLike
Thank you Amanda for “laying it all out there”. I appreciate your candor and all the detail you share in this fight with cancer. You are such an inspiration. Love you!
LikeLike
Bless you sweet girl! I am sorry you’re going through such a challenging time. I am amazed at your bravery and am sending all kinds of healing energy! Be kind to yourself and take the time you need to heal!
LikeLike
Amanda, Katie had told me about your diagnosis awhile back. When I checked with her on your surgery, she sent me the link to your blog. I am so impressed by your strength, fortitude and courage as I’ve read your posts today. I am praying for you and your family as you make this journey.
LikeLike