Hi! It’s been forever. I just scanned my most recent post and WOW- a lot has happened since then (I think I say that every time I post here, but this time, I REALLY mean it) It’s now January 2024. It’s been about a year and a half since I last posted. I’ve gone through clinical (4th) year of vet school, graduated with an entirely new (wonderful) Class of 2023, become a doctor, had my reconstructive surgery, lost my sweet Frankie unexpectedly, traveled a bunch, adopted a puppy, had a 5-day hospital stay that resulted in losing my left breast implant just before starting my new job as a vet, and a whole bunch of other stuff. Undoubtedly, the hardest part of the last year and a half was having to say goodbye to my soul dog, Frankie. If you want a rundown of everything that happened with our sweet big guy, read ahead…if you’d rather skip the sad stuff and stick to cancer/other updates only, skip this next section.
Frankie had lymphoma which we didn’t discover until he was having some severe hind limb weakness/shaking while I was volunteering at a spay/neuter trip in Montana in June. I brought him into CSU for a workup with orthopedic medicine, neurology, and some bloodwork to see what was going on, and while in the hospital that day, a friend noticed that his breathing seemed a bit labored (he had also been more reluctant to go for longer walks since I had returned from the volunteer trip, so we knew something was up). We did a bedside ultrasound in urgent care (thanks to my amazing ER wizard friend Dr Cavanagh) and she found quite a bit of fluid surrounding his lungs (almost 2 liters). We drained the fluid and looked at it under the scope, and it had the type of cells that are indicative of lymphoma. We then did a full ultrasound the following day and sure enough, many of his internal (GI) lymph nodes were quite enlarged. We took some aspirates of his liver and spleen and he was diagnosed with a rare form of lymphoma that even CSU’s oncology department didn’t know a lot about. He was in the ICU when I was having reconstructive surgery, and Brandon brought him home from the ICU the day I was released from the hospital. We spent a few special recovery days together before he very quickly went downhill due to the high dose of steroids he had to be on to slow the cancer. Options for canine chemotherapy had unknown outcomes and would have prolonged his pain and suffering likely to only have a few more weeks with him, since the type of lymphoma he had was not well understood and they weren’t sure how he would respond to chemo, or whether it would make a difference. Ultimately after a few days of watching him decline very quickly, I knew in my gut that it was time to say goodbye to Frankie’s earthly body. My best friend and Frankie’s very favorite Auntie Danni was able to help him pass over the rainbow bridge peacefully at home, while we cuddled together after she gave him a McDonald’s cheeseburger, which was probably the best moment of his short life. I still haven’t been able to bring myself to fully process his loss. It was during such a wild and stressful week with my own surgery, and it was such a quick decline…I’m grateful that we were able to give him the gift of a calm, painless passing, but I don’t know that I’ll ever understand why these things happen to creatures like him. I have never known a purer soul than Frankie. He had such a hard beginning with neglect and abuse and lived such a short life. But in that short life he gave more love than I knew possible. I will forever be beyond grateful that he was ours for three years. It will never ever feel like it was long enough. Giving Frankie our hearts and a loving home is one of the greatest joys of my life. I miss him in a deep, profound way that I still can’t put into words. Photos of him are all around my place and we have his ashes in a beautiful bamboo urn on my healing plant shelf. I kiss it goodnight every night and I wish more than anything I could kiss his sweet chops again. Someday I’ll be able to scroll through his photos without crying, but for now it still feels like a stab to the heart when I let myself really think about him. I feel so incredibly lucky to have been blessed to be his mama.









Ok, whew. I started this post three months ago and had to stop and revisit this section in public at a coffee shop to get through that and ensure I didn’t start crying and walk away from it again…
I finished vet school! 4th year was insanely busy and very tiring but actually a lot of fun. There were some imposter syndrome moments for sure, but overall I really enjoyed it- even my horse girl rotations, which I did not expect. Below are some random photos from 4th year that feature some patients from rotations at CSU and some externships. I officially enjoy doing surgery (NEVER would have thought that when I didn’t even know how to hold surgical instruments a few years ago) and still love conservation medicine, aquatic medicine, shelter medicine, and affordable access to care (aka spectrum of care/low cost medicine/etc). I was fortunate enough to be able to do some incredible externships amidst having to take 9 months of medical leave from school for cancer treatment. I spent two weeks working with the vets at Vancouver Aquarium, spent a few weeks with the vet and my dear friend Dr. Joyce Thompson at the Wild Animal Sanctuary working with tigers, bears, lions, and other large predatory species, and had an incredible few weeks back in one of my very favorite countries, South Africa, working with two conservation vets doing rhino dehorning, elephant collaring, and relocating zebra, wildebeest, and impala. Needless to say, it’s been a busy year and a half. My sibs, some close friends and I also traveled to the Pantanal and Rio de Janeiro, Brazil this past August which was absolutely phenomenal. I feel so lucky to have been able to do all of these things while recovering from surgeries and during ongoing treatment.








A few cancer-related updates, since that’s what we are (mostly) here for:
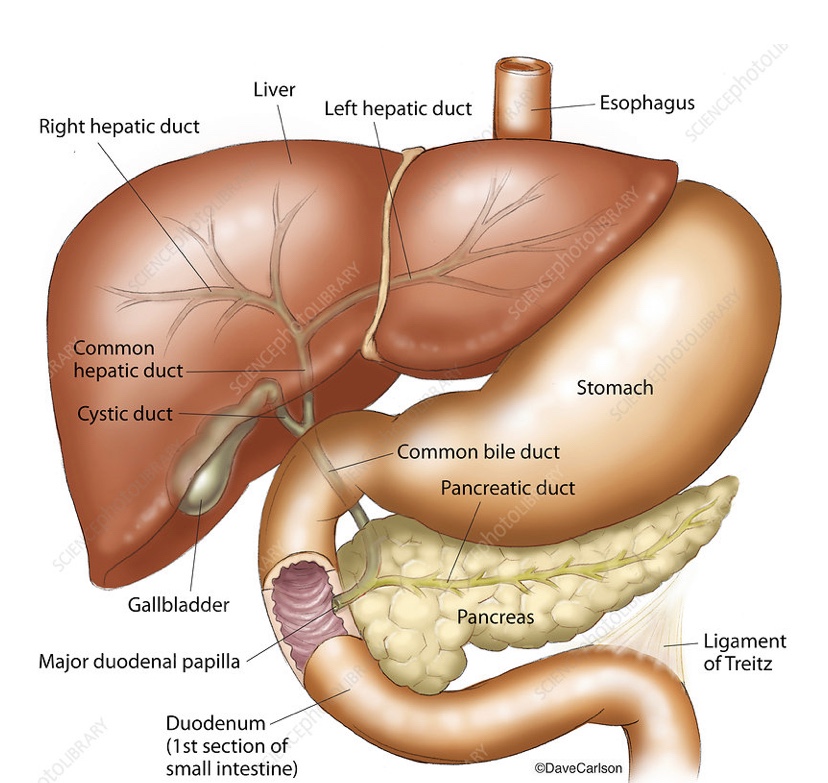
- Reconstruction happened June 15th (they changed out my expanders for implants after over a year of having the expanders in). I healed well from this surgery and was pretty happy with the results, all things considered. Giant scars and no nipples, as most of you know by now, but overall things looked as good as they could have considering having both breasts, 15 lymph nodes, my left liver lobe, and my uterus and ovaries removed, 40 or so chemo infusions over a year, 33 rounds of radiation, skin stretching, 1 year of expanders, and then an exchange surgery for the “final” implants (“final” in quotes because…well, you’ll see).
- I traveled to Africa and Brazil a few weeks after surgery for about one month total (2 days at home in between locations) and for the most part had no issues. I had a few days of a very minor infection in my incision line where my skin was radiated (where the original tumors were, high up in my left breast). The infection cleared with antibiotics and didn’t affect my travel much at all, beyond the last day or two in Brazil when a 5-mm section of my incision line seemed to have opened up a bit.
- When I returned home, I had my 3-month post-operative appointment at Anschutz, which actually turned from a post-op “you should be fully healed by now” appointment to “hmmm, that part of your incision that keeps scabbing over is concerning, let’s just remove that scab and see what’s going on underneath” appointment.
- The subsequent “oh shoot, now we can see your implant right underneath that area we just removed so we should probably put you back on antibiotics and stitch it back up and hope for the best” led to sepsis less than 24 hours later.
- Brandon and I went to Beetlejuice the musical at a fancy theatre in Denver the night after they stitched my incision back up, and I felt like absolute shit (but the show was fantastic!) Turns out that’s because I was getting infected and going septic.
- Sepsis led to an ER visit the next morning, emergency implant removal surgery, wound vacuum placement for three days, IV antibiotics, a failed attempt at putting implant back in by my surgeon, and then waking up from the second surgery, being told my left breast implant could not be put back in due to inflammation and skin integrity and we have to restart the reconstruction process with a much more invasive surgery starting sometime in 2024.
- Not ideal
So, where are we now? And what’s next?
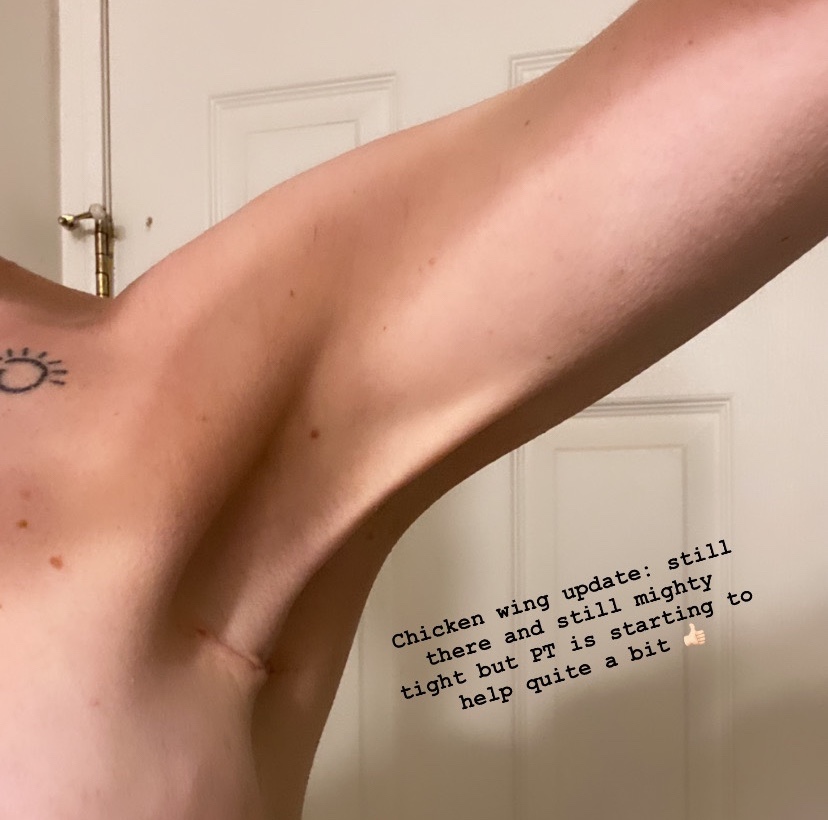
My next surgery will be a “lat flap” (latissimus dorsi flap) and will take place this coming July (so 7 months from now). This means my surgeon will have to take a portion of my latissimus dorsi (“lat”) muscle on my left side/back and underneath the skin they will pull it in front where my breast should be and use the vasculature from this muscle bed to aid in healing over the top of a new expander they’ll place at the same time. This is because my previously radiated skin “failed” to heal properly over the implant on my left side (honestly I think had I not gone to that 3-month recheck and had they not opened up that tiny little scab and then restitched my incision that day, I think it would have eventually healed and I would still have both breasts reconstructed, but I try not to dwell on that). The lat flap surgery has a very high success rate (~95%) but is generally only used as a “salvage” procedure when other more straightforward/less invasive reconstructive surgery methods fail. There is another option called a “deep flap” where they take belly fat and bring it up to your breast area to aid in reconstruction, but since I don’t have a lot of fat on me my surgeon has indicated several times that this would not be a very successful method unless I gained ~30 lbs (this I definitely don’t want to have to do because I want to stay as fit as possible to help my body heal and keep this nasty disease at bay). So, lat flap it is. I am a little bummed since it reduces strength on that side, but with proper physical therapy and continued active lifestyle I can regain the majority of my strength (usually to about 80-90% previous strength) and range of motion on that side if I work hard at it. I will always be a little uneven as they have to pull a significant portion of that muscle forward, and my friend who has had this surgery in the past has indicated that it feels really weird because whenever your back muscle flexes, you feel it on your breast, but at this point I don’t really have any other choice. I definitely still want to pursue reconstruction since I am young and (hopefully) have a lot of years ahead of me, but if this one fails, we’ll see. My surgeon said usually if this type of surgery fails, they stop reconstructive efforts. So fingers crossed this one works and holds and we don’t have to do too many more revision surgeries after the final implant exchange, which would take place about 3-6 months after the July surgery.
I have been wearing a breast prosthesis in mastectomy bras for the past few months and it works fine with regular shirts and some tank tops, but I don’t want to have to wear one forever, especially if I am in a swimsuit/bikini or sports bras working out. They’re fine, just annoying to have to put in a bra every morning and can get heavy and take some pinning, etc. when I am trying to dress up in cute outfits for shows or going out. I’d much rather just have a real(ish) looking breast back! The recovery from this type of surgery is estimated to be about 6 weeks, so I’ll have to take short-term disability from work. As mentioned above, ~3-6 months after the lat flap, once my skin is stretched out again over the expander (and as long as everything heals properly), I’ll get an implant exchange surgery.
Other cancer/medication/chemo updates: I am still on daily Anastrazole to reduce the estrogen released from my pituitary gland since my type of cancer responds to estrogen and we don’t want any in my system these days. This leads to joint pain which I am semi-used to but causes a moderate amount of pain when I sit for more than ~30 minutes or if I run/do Pilates/yoga/biking without proper amount of stretching and anti-inflammatories. I’ve learned to live with the chronic pain, but I look forward to ~4-8 years from now when I can be done taking Anastrazole (most women take it 5-10 years depending on their disease). Every 6 months I still get infusions of Zometa, which helps with bone strength since the lack of estrogen in my body leads to osteopenia and possible osteoporosis if I don’t take calcium and manage bone health with scans once per year. Running and strength training are also very beneficial which I try to do regularly. I try to balance running 1-2x per week with Pilates and yoga, which helps my joints from too much pavement pounding but I do still love to sign up for races and hope to be able to continue half-marathons for at least the next decade or so if my body allows.
I started a new oral chemotherapy called Nerlynx this afternoon. It makes you poop your pants. I can’t wait to start this and try to balance it with hectic 11-hour work days and being scrubbed in doing surgery and in 15-20 appointments a day with stressed out clients and their pets in exam rooms. It’s going to be interesting! I have 200 Imodium prescribed to me to help with the diarrhea that is imminent. Other side effects are similar to previous infusion chemo side effects, but hopefully not as common- nausea, dry skin, runny nose, weird nails, face and hand/feet rashes, vomiting, lethargy, dizziness, etc. etc. etc. etc. etc. etc.
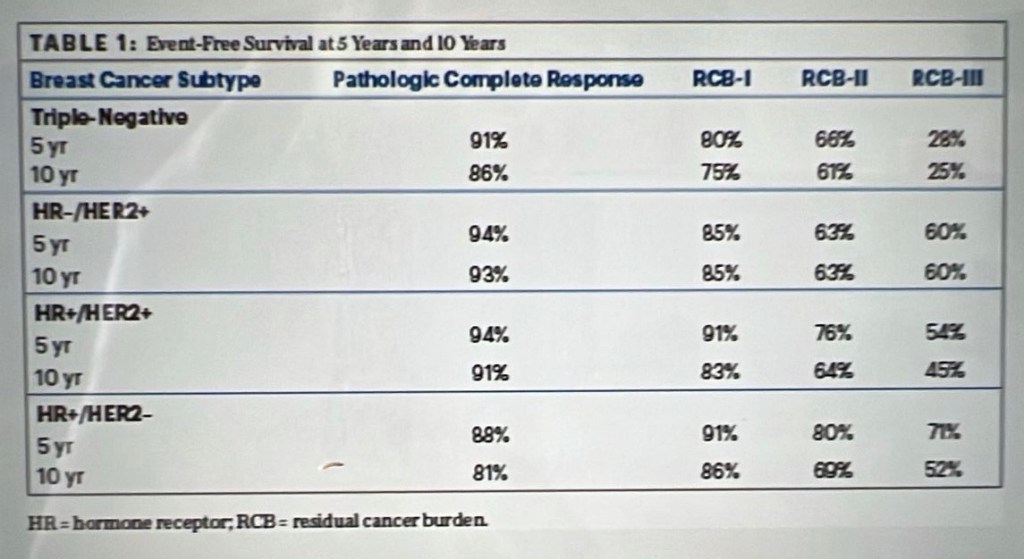
I am supposed to take this medication for one year, so 2024 may end up being the year of the adult diaper. This medication is supposed to reduce the chance of metastasis to the brain, since the type of disease I have (triple positive, which includes the HER2 protein) likes to travel to the brain. To assess my tolerance to this medication, I have an appt with my oncologist or my oncologist’s NP every two weeks before they increase the dose. Week one starts with three 40-mg pills, week two is four 40-mg pills, and by week three I should be at six 40-mg pills a day. I know one friend who was able to tolerate it and get through the whole year but had to strategically plan outings and work obligations to ensure bathroom availability, and another friend who could not tolerate the medication well enough to be able to leave her house without experiencing emergency scenarios. So, we’ll see how this shakes out. I’m hopeful, but not necessarily optimistic.
I have a brain MRI in two weeks to assess whether the mass they found in my brain upon diagnosis is stable or has grown. Fingers crossed it’s a benign pituitary adenoma, but if it’s grown then we have some other problems to address. My prolactin levels are a little higher than they should be (this is one of the hormones released by the pituitary gland), especially after being in forced menopause for over two years now, so they want to make sure it’s not coming from this mass.
Work updates:
I have been Dr. Vegter for a bit. Still getting used to being called Doctor by all of our techs and assistants and clients, but it’s feeling more real and more digestible with each passing month (although I prefer if they just call me Vegter). I love doing surgery and seeing (most) patients, dental extractions are still hard for me, but I am learning quickly, and I am enjoying my team a lot. I work for a giant corporate clinic which has its benefits (pay and healthcare and consistency of work) but also its limitations/downsides (always pushing for higher caseload which can be super stressful and sometimes leads to compromised care, which I really don’t like). However, the high caseload does help me learn to balance chaos and pushes me to make quick decisions, can benefit more patients/owners since we see A LOT every single day, and this will be helpful once I move back over into the NGO world and start a rescue (or partner with a current rescue after a few years in corporate), since rescues are so inundated with animals right now because people keep breeding and breeding and not getting their animals spayed/neutered and the overpopulation problem is insane. So, there will never be a lack of animals in need coming into rescue, and caseload will always be high. Still TBD if I’ll want to pursue rescue/shelter medicine here in Colorado or move abroad for a year or two (if I am healthy and can do this, Brandon and I definitely want to try) and do some rescue work in a place of high need (which hopefully can include some aquatic medicine/rehab as well). That will probably be in the 5-year plan, maybe a bit longer. I do really like my current clinic and my mentors and manager, and overall, it’s been a good experience so far. Just have to keep learning and working hard and trying to manage the stresses of work with cancer treatment and a few more surgeries.
Other life/kiddo updates:
Meli is doing great. She is 8. She is my best girl and I love her with every ounce of my soul. She continues to be my guiding light and gives me so much purpose and brings all sorts of happiness on the daily. Bodie is our new addition, and he is a little stinker and soooo naughty but I love him with all of my heart also. He is in crazy shark puppy mode every single day and has already cost me $5000 for a foreign body ingestion and aspiration pneumonia (thank god for pet insurance which reimbursed me half of this cost- GET PET INSURANCE!!!) but he is still perfect and he is the best boy in his kennel for long days when I am at work. His dog walkers agree he is naughty but luckily he is super cute and doofy so they love him too. Our angel boi Frankie is always here with us and I try to honor him every single day by helping doggies in need through my work as a vet and taking the best care of his big sister and new little bro.
Brandon and my family continue to be extremely supportive and awesome in helping me through the chaos that is this phase of life. Brandon is working hard as always to be the best dentist to his patients, mentor to his new associates, son/brother to his family, and partner to me. He is an amazing companion, and we continue to strive to adventure, explore, dance, party with our awesome friends, and live that Breck cabin life whenever possible. We are very fortunate and continue to work hard to keep our lives meaningful, fun and interesting despite the challenges we’ve faced over the past couple of years. We realize that despite this cancer nonsense, we are still incredibly lucky to have what we have and so many people in this world are experiencing hardships that we could never fathom, so we try to be grateful and hope to give back in a bigger way once we have time to do more volunteer work in the US and abroad.
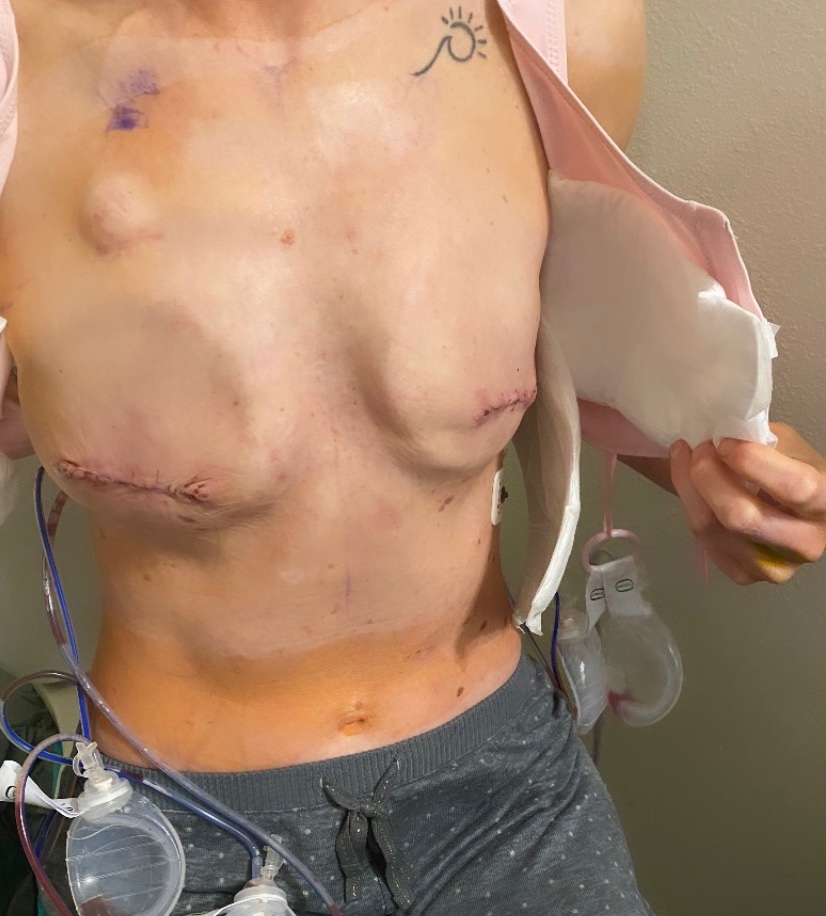
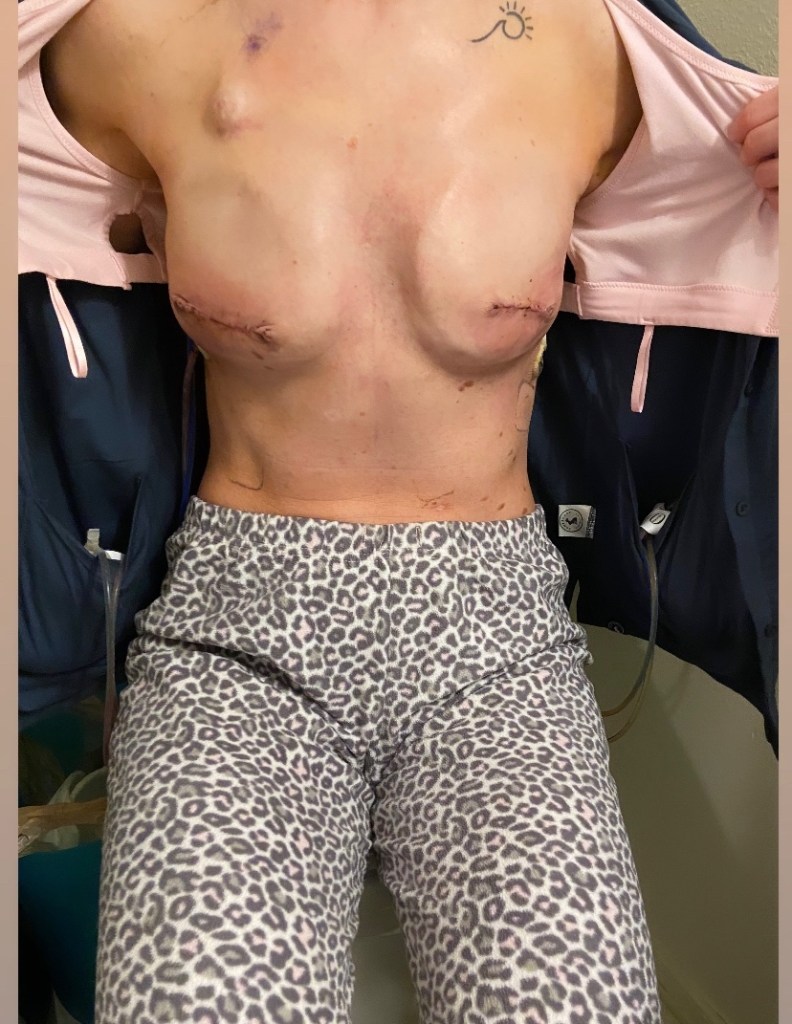
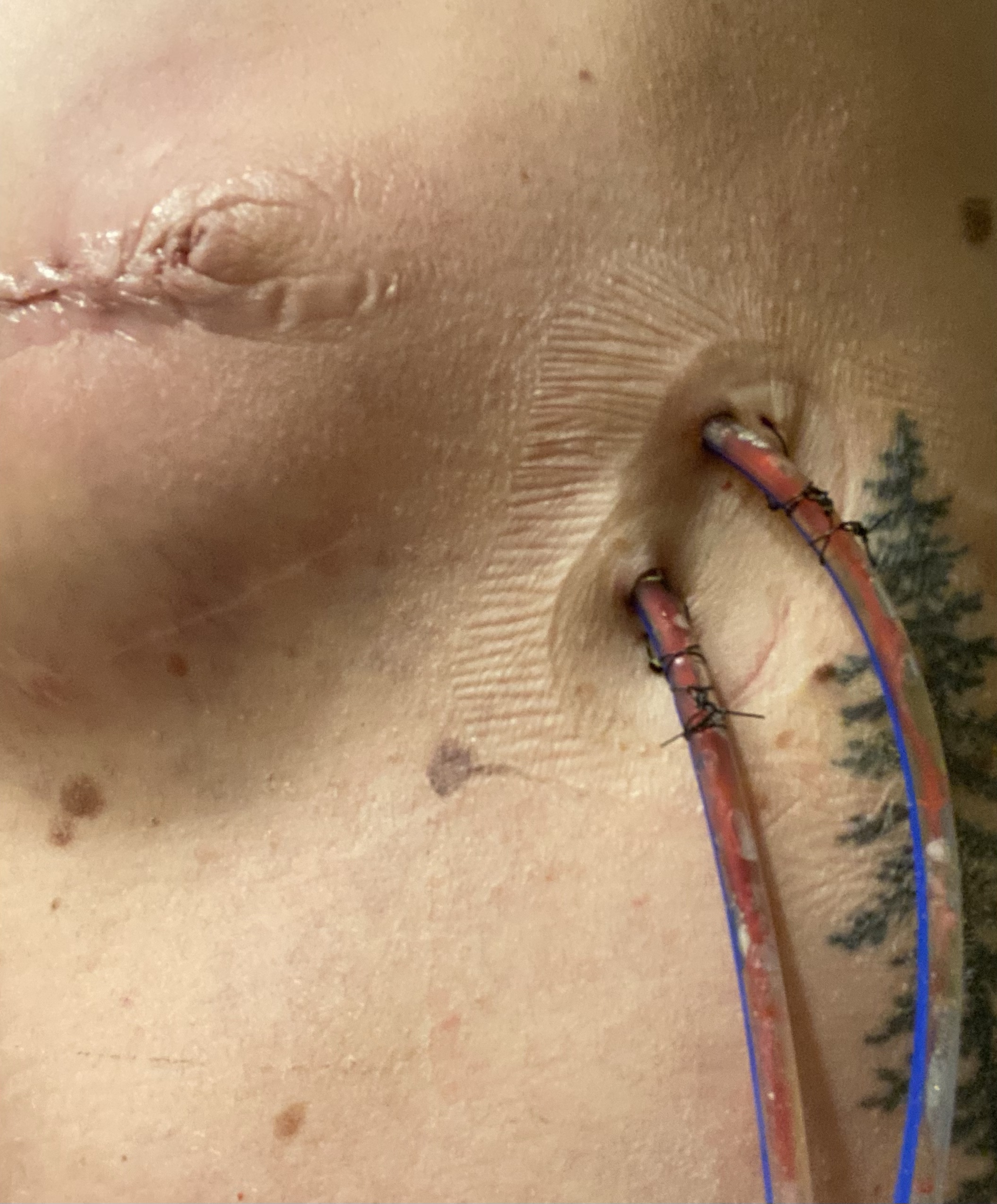
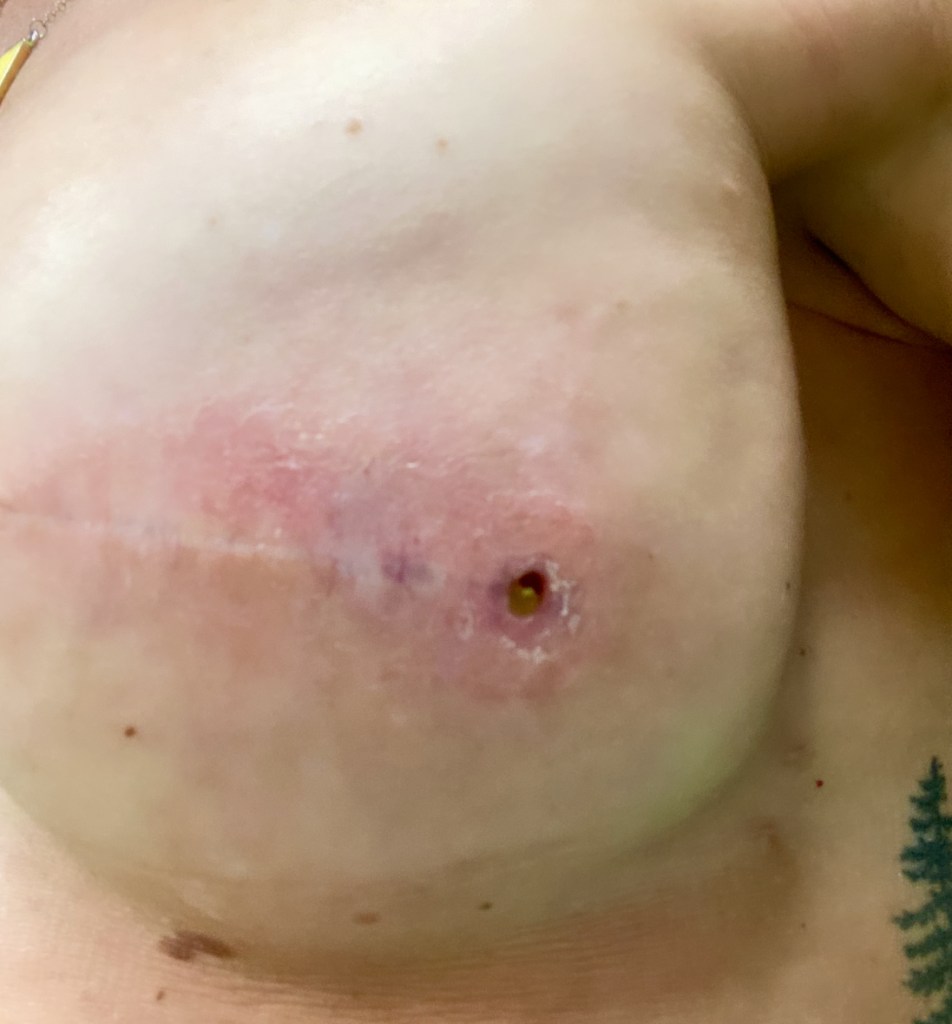
Below are some photos of what my incision looked like about 1.5 months after my first reconstructive surgery (the third photo) and then how it looked after about 2.5 months when they removed the little area that wouldn’t heal and stitched it back up at my 3-month recheck appointment (this is what led to the infection and hospital stay).
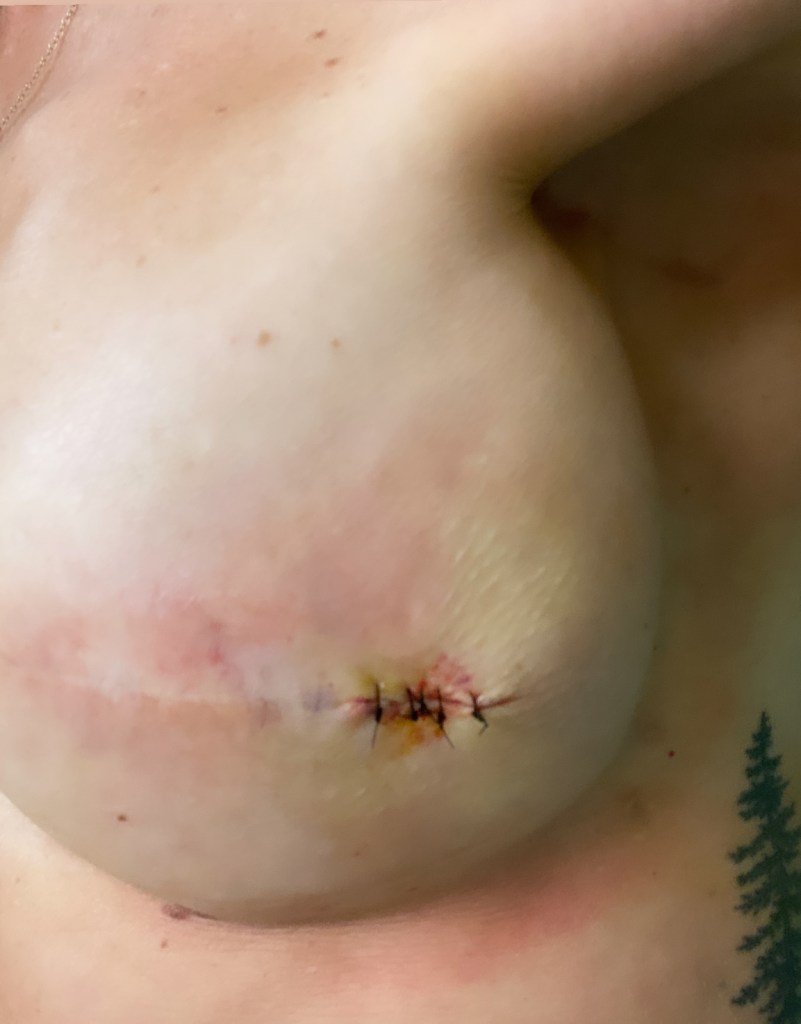

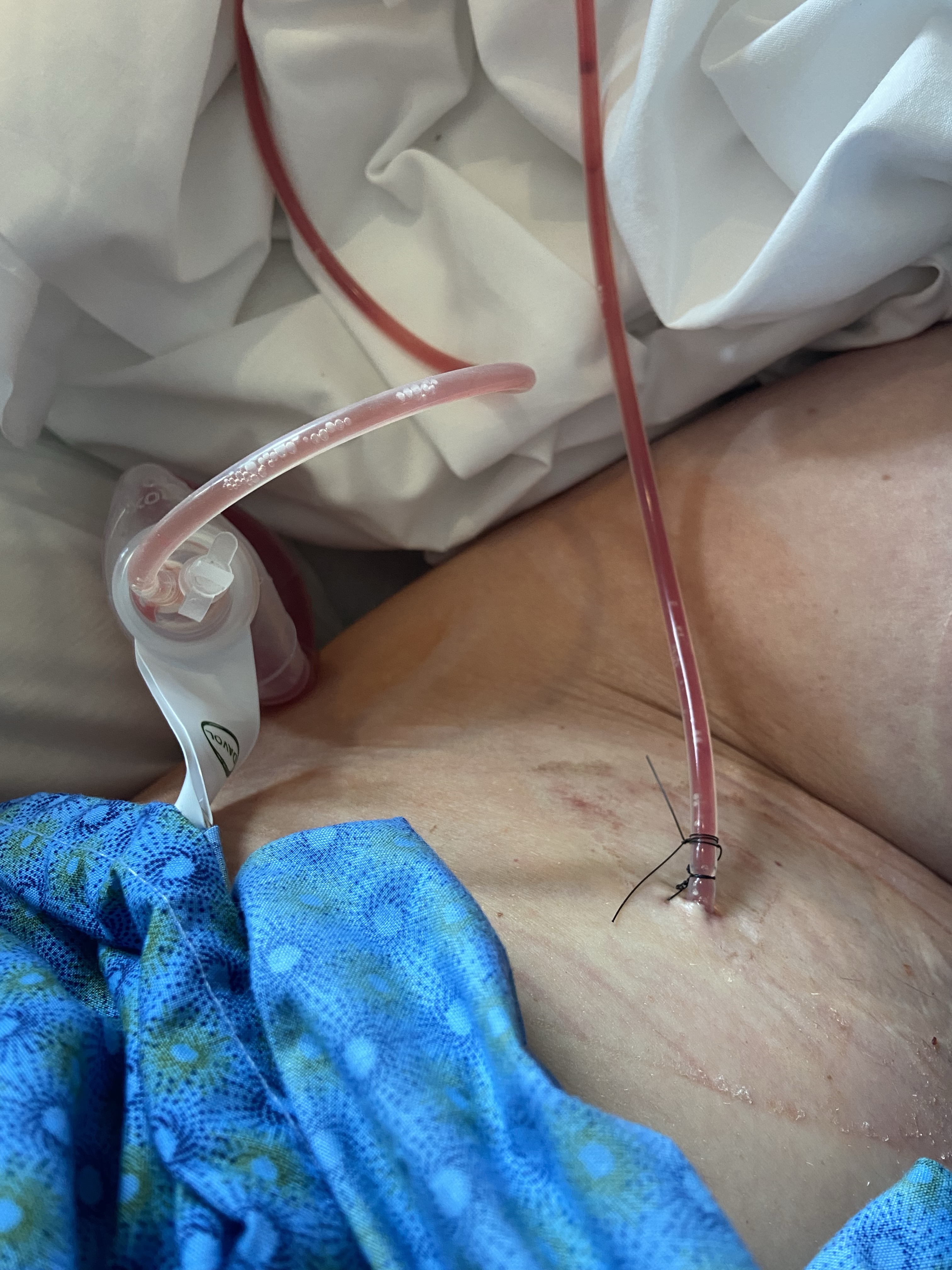
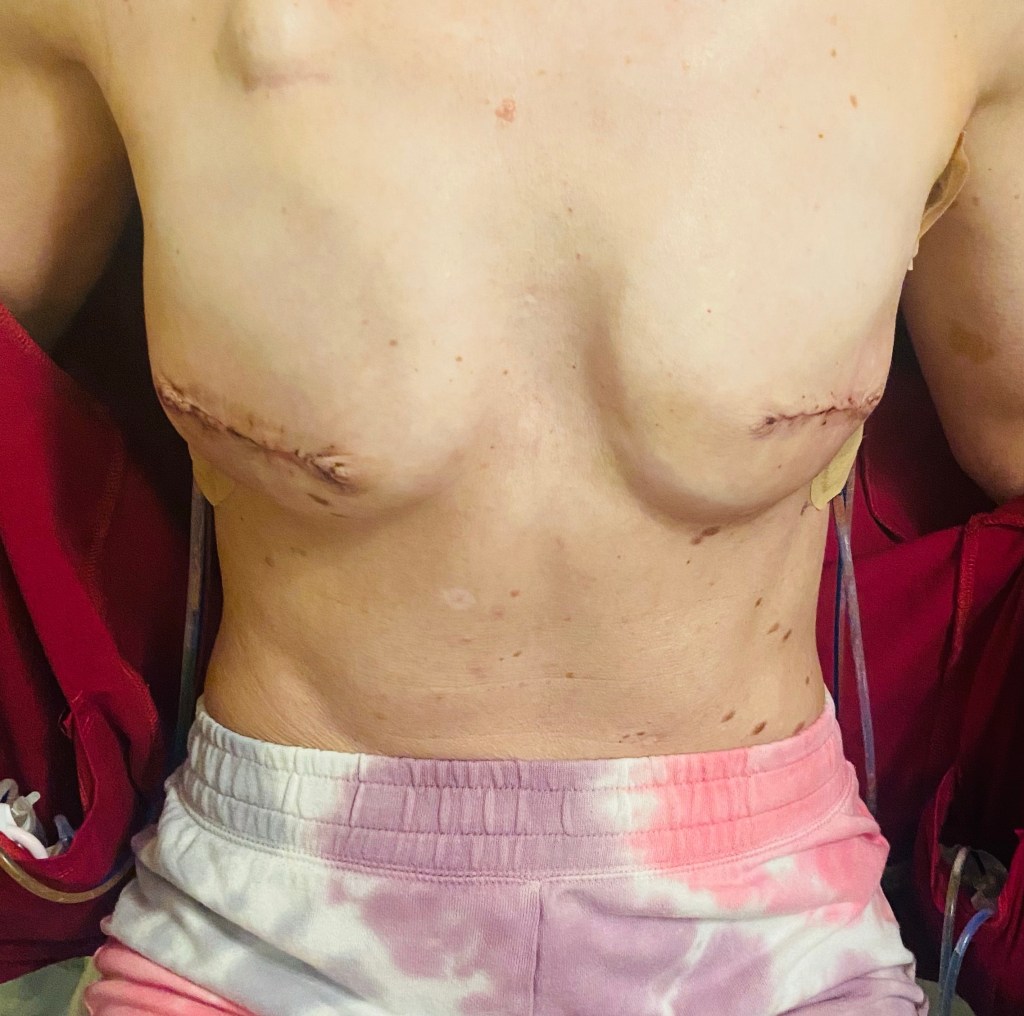
The photos below are what things turned into during my emergency hospital stay when they removed my left implant, placed a wound vac for a few days, then removed the wound vac and attempted to iput a new implant in (which failed), which resulted in no breast on the left. The last photo shows how things have healed up since then.
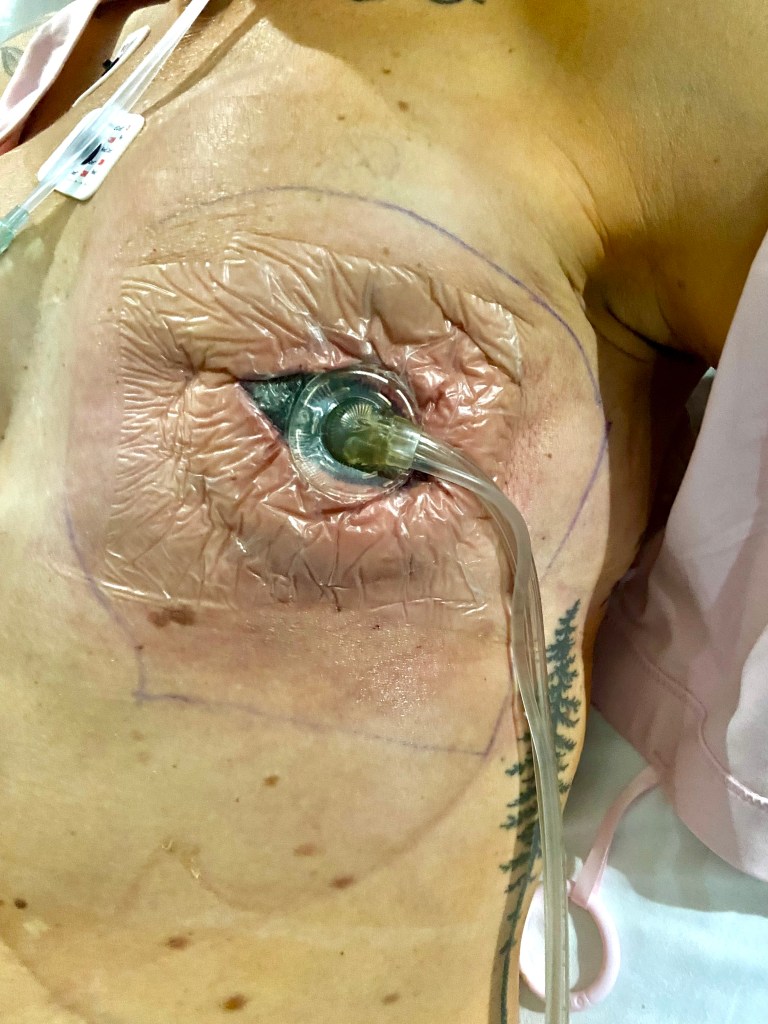

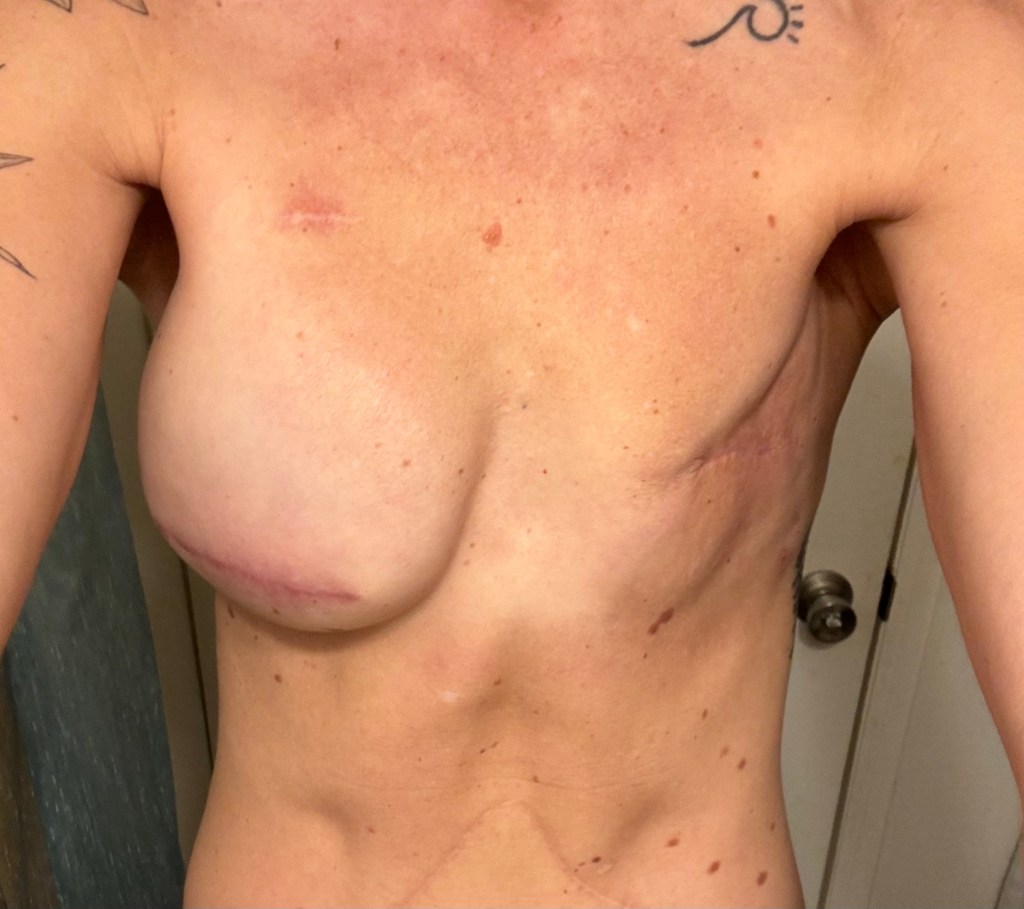
And as always, some (better and less creepy) photos of fun times amidst the chaos of life with cancer.










































Thanks for sticking with me for this very long (and way overdue) update, and as always, I appreciate everyone’s support from all over. Please feel free to reach out to me with any questions if anyone reading this is going through something similar or knows someone else who is and needs to talk to someone who knows what it’s like.
Sending love and doggie kisses to everyone!